An R on T premature ventricular complex (PVC) is an important concept in ECG reading as it may lead to ventricular tachycardia, ventricular fibrillation, and possibly sudden cardiac death. Recognizing an R on T PVC on a rhythm strip may save a patient’s life.
What is an R on T PVC?
Let’s not beat around the bush. Simply stated, an R on T premature ventricular complex means that a QRS complex from a premature ventricular beat lands on the preceding T wave. That’s it. So what is the big deal? Unfortunately, this condition can set the patient up for life-threatening arrhythmias. The most common is polymorphic ventricular tachycardia.
What Does R on T PVC Look Like
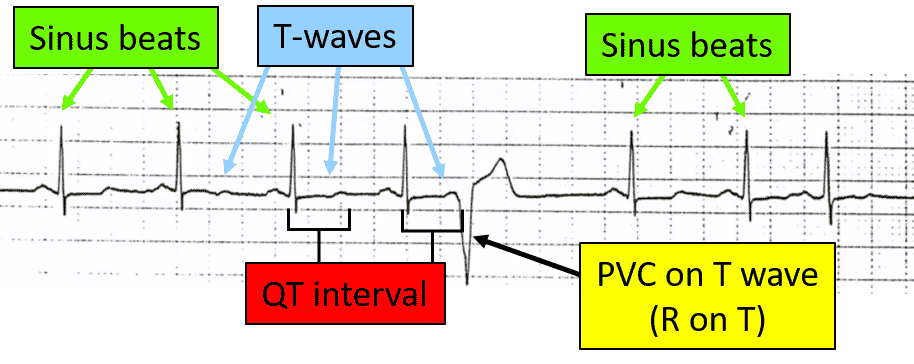
Here are some examples of R on T premature ventricular complexes. The first one is a PVC that fell on the T wave of the prior beat but did not lead to an arrhythmia. The next two examples show a PVC that again landed on the preceding T-wave and put the patient into ventricular tachycardia.
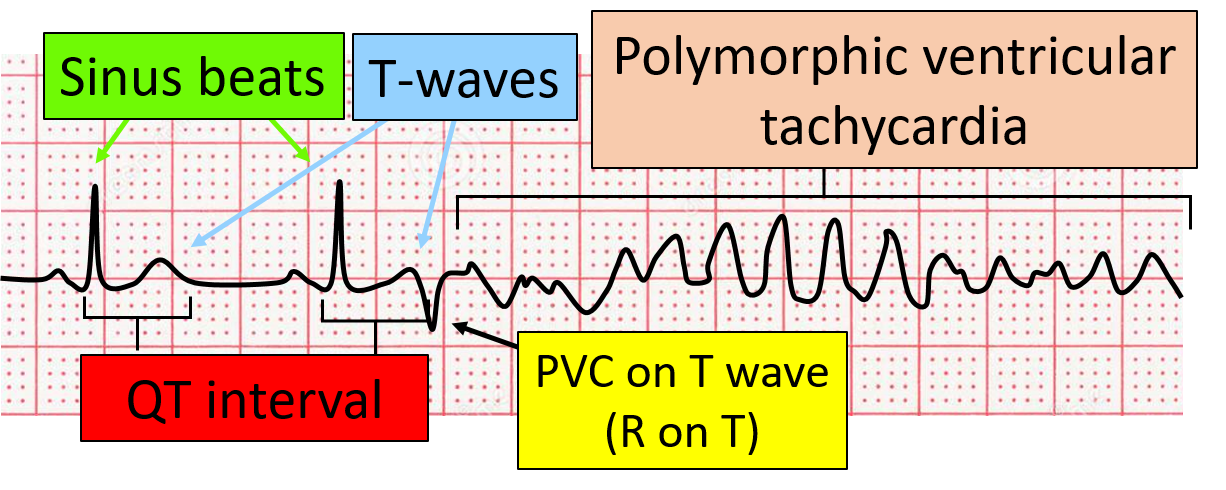

What Are the Consequences of R on T PVCS?
Because of the timing of this premature ventricular complex, patients may develop polymorphic ventricular tachycardia (PVT). PVT in itself impairs cardiac circulation and may lead to syncope (passing out) or death.

Start Your Membership Today
We make electrocardiogram interpretation simple and understandable. The videos are interactive, and have detailed, easy to follow illustrations.
What is the pathophysiology of R on T Premature Ventricular Complexes?
Since all cardiac tissue has the ability to produce spontaneous beats, premature ventricular complexes (PVCs) occur when a piece of the ventricular tissue suddenly becomes active. The exact reason for PVCs is unknown, but may be exacerbated by stimulants such as caffeine, catecholamines, anxiety, electrolyte imbalances, or certain drugs.
Action Potential of Muscle Cells
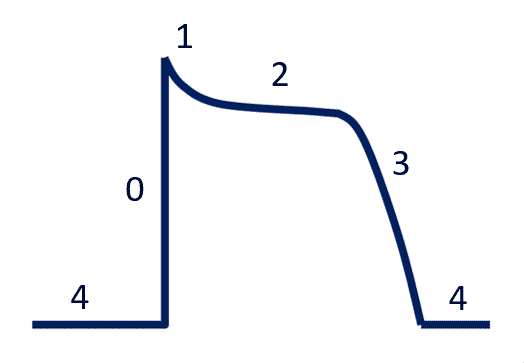
Now let’s back up a little and look at the action potential curve for muscles. There are 5 phases (Phase 0 – Phase 4). The details of these phases are not so important, but rather the timing of the placement of the PVC is. You can look at the diagram below for more details.
Action potentials and impulse conduction
- Phase 0: Depolarization (rapid influx of sodium)
- Phase 1: Early repolarization (efflux of potassium)
- Phase 2: The plateau phase (influx of calcium through slow calcium channels and continued efflux of potassium through delayed rectifier potassium channels)
- Phase 3: Rapid repolarization (calcium channels close, but continued efflux of potassium)
- Phase 4: The resting phase (no ionic activity; steady state)

Start Your Membership Today
We make electrocardiogram interpretation simple and understandable. The videos are interactive, and have detailed, easy to follow illustrations.
Alignment of the Action Potential and ECG Waves
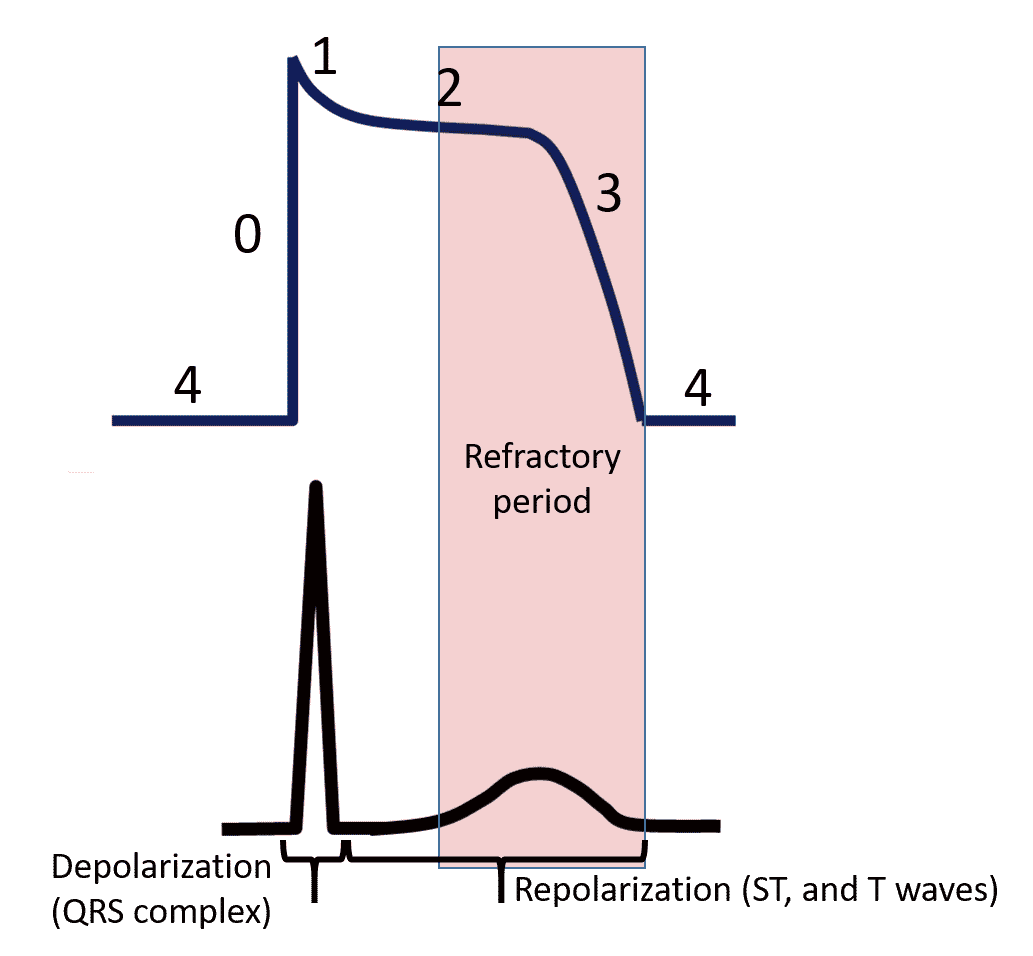
Look at the picture below. You will see that the QRS complex lines up with phase 0, depolarization and that the ST and T waves line up with repolarization, phases 1, 2, and 3.
The Basic Concept of Reentrant Tachyarrhythmias
For simplicity, there are three basic components needed to produce a reentrant arrhythmia.
- Two pathways
- One of the pathways is slower than the other
- A unidirectional block
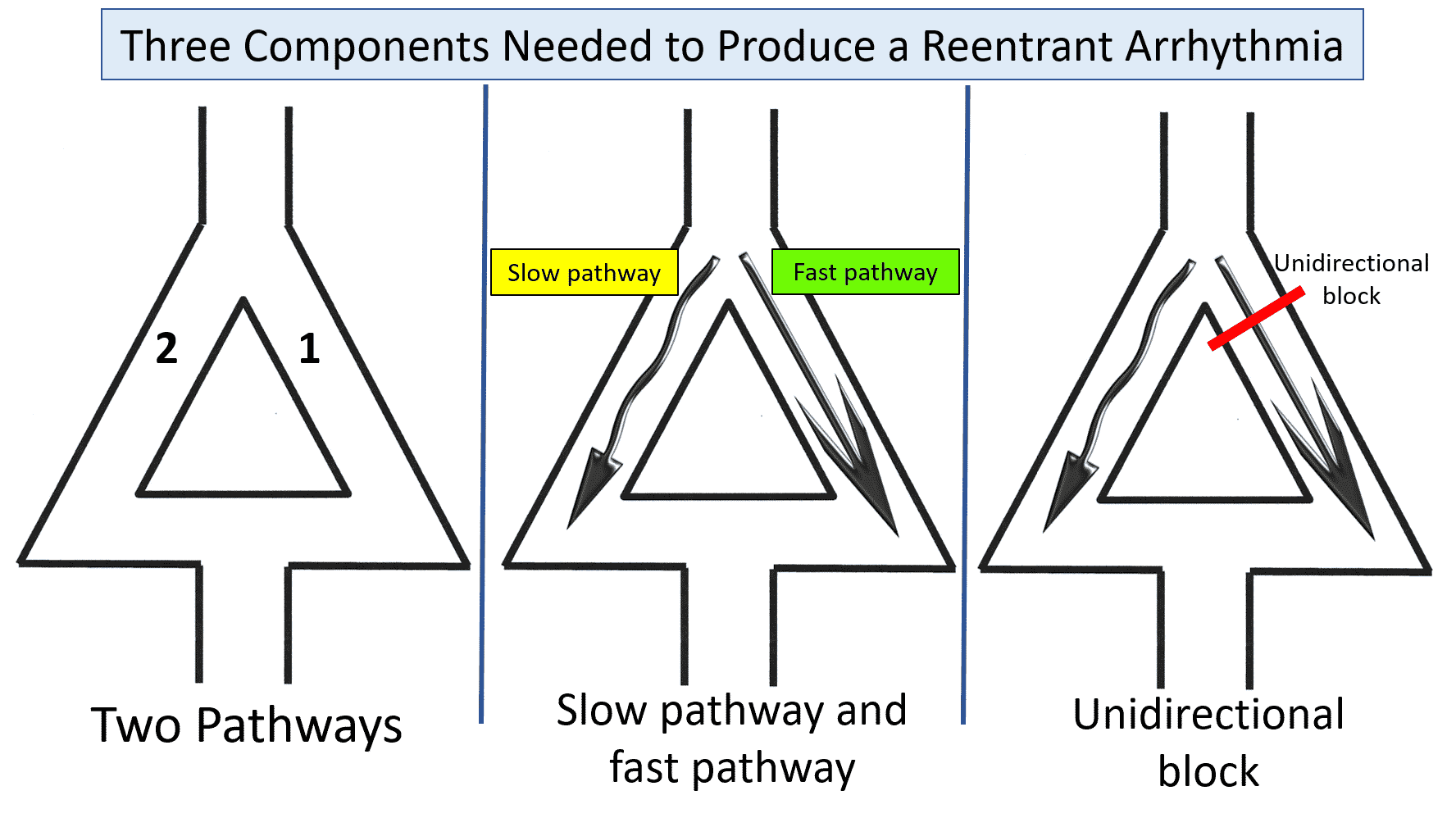
The diagram below is typically used for demonstrating this. To begin, you see two pathways. The right side depicts the fast pathway that typically conducts impulse. The left side represents the slow pathway. Impulses may start down the slow pathway but are stopped at the bottom since the fast pathway, which has already depolarized, is now refractory. The third factor, or unidirectional block, is brought on by a premature beat.
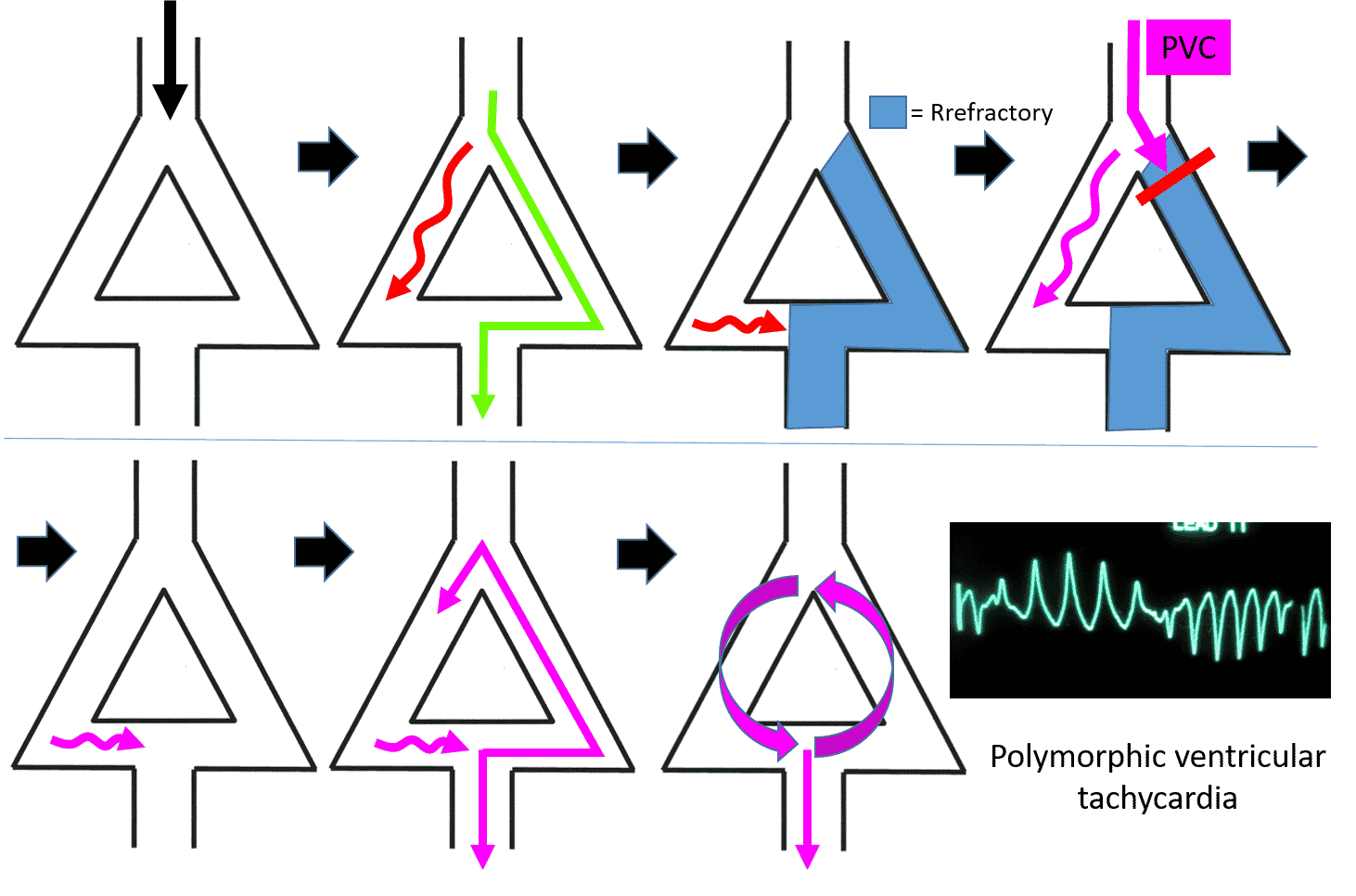
We’ll say that an impulse is traveling through the ventricle and stimulates this area of cardiac tissue. This impulse excites both the fast and slow pathways together. The impulse speeds down the fast pathway to stimulate the next set of ventricular cells. The fast pathway now is refractory (cannot conduct) and is in stage 3, repolarization.

Try Our ACLS Rhythm Course For Free!
This course goes through all of the ACLS rhythms. You will be quizzed on each rhythm and then watch the detailed description which points out the salient features.
Remember that the slow pathway had also been stimulated. This impulse travels down the slow pathway and stops when it gets to the intersection of the fast pathway because the fast pathway is refractory.
Let’s imagine now that a premature ventricular complex comes down and try’s to stimulate this area of ventricular tissue. When the impulse tries to go down the fast pathway, it is blocked because the fast pathway is still refractory from the previous impulse. This is our unidirectional al block.
The PVC’s impulse, however, can go down the slow pathway. This PVC impulse does, however, meander down the slow pathway. By the time the impulse gets to the fast pathway, the fast pathway has repolarized and is able to conduct the impulse.
This impulse not only stimulates the ventricular tissue causing another PVC, but travels up the fast pathway allowing it to set up an impulse loop that continues down the slow pathway, causes another PVC, and circles up the fast pathway again. Once up the fast pathway, it again stimulates the slow pathway and a circular electrical current is set up. Every time the impulse hits the bottom of the slow pathway, it causes a PVC. Every time it goes up the fast pathway, the cycle recurs. This results in ventricular tachycardia.
How an R on T PVC Causes Ventricular Tachycardia
Most PVCs do not cause a reentrant tachyarrhythmia. The PVC itself is not the problem, but instead, it is the timing of the PVC.
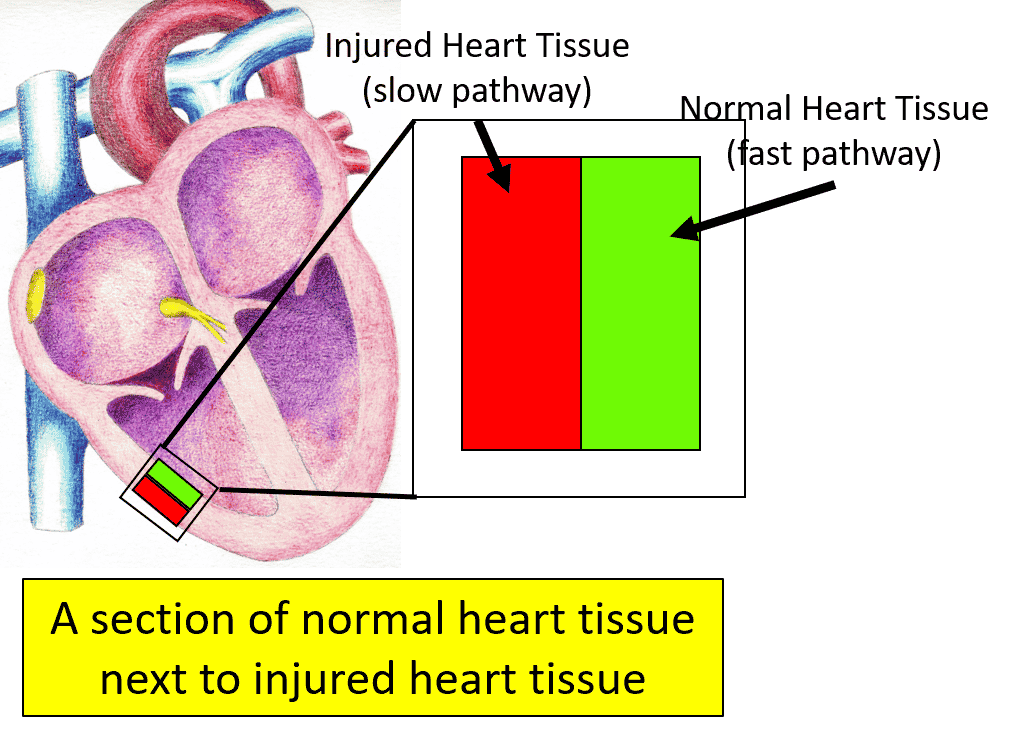
Imagine that there is ventricular tissue that is injured, and sits next to normal ventricular tissue. We now have two pathways for an impulse to travel. Since one of the pathways is from injured ventricular tissue, then the conduction is slower than the normal tissue. As you see, we now have two of the conditions needed for a reentrant tachyarrhythmia (two pathways, with one of them a slower pathway). All we need now is a unidirectional block.
A PVC landing on a T wave now hits the normal tissue (fast pathway) when it is refractory (unidirectional block). The PVC’s impulse can now travel down the injured ventricular tissue (slow pathway). By the time this impulse reaches the normal ventricular tissue (fast pathway), it has repolarized and is ready to conduct. This impulse then goes up the normal tissue, back down the injured tissue and our reentrant circuit is set, causing ventricular tachycardia.

Try Our ACLS Rhythm Course For Free!
This course goes through all of the ACLS rhythms. You will be quizzed on each rhythm and then watch the detailed description which points out the salient features.
How to Treat Patients with R on T PVCs and Possible Ventricular Tachycardia
Treating patients with this condition requires preventing ventricular tachycardia from occurring in the first place. If ventricular tachycardia does occur, a completely different approach is needed. For preventive treatment, I think of ways to treat the three conditions needed to produce the reentrant arrhythmia in the first place (two pathways, a slow pathway, and PVCs).
Treatment for Ventricular Tachycardia
Once the patient is in ventricular tachycardia the patient needs emergent shock therapy or antiarrhythmic medications.
Treatment for the Two Pathways
Electrophysiologists (cardiologists who specialize in the electrical system of the heart) can sometimes perform a procedure called ventricular ablation. During this procedure, the electrophysiologist runs a wire into the heart through the patient’s vein, localizes the abnormal tissue, and applies electricity, heat, or cold to the ventricular tissue. This essentially gets rid of the second pathway, which prevents the reentrant arrhythmia from occurring.
Treatment of the Slow Pathway
Various treatments are used to alter the speed and sensitivity of both the fast and slow pathways. Medications may include beta blocking agents or antiarrhythmic agents. Patients may need electrolyte replacement or medications to optimize their electrolyte levels (e.g. potassium, magnesium, and others). Patients should avoid substances and medications that may stimulate arrhythmias (e.g. cocaine, decongestants, and others). Medications that prolong the QT interval (the section of the ECG waves representing repolarization of the ventricles) should also be avoided.
Treatment for Premature Ventricular Complexes
Since the exact etiology of PVCs is unknown, the exact treatment is also unknown. Certain agents like the ones above which affect the pathways also may reduce PVCs.

Start Your Membership Today
We make electrocardiogram interpretation simple and understandable. The videos are interactive, and have detailed, easy to follow illustrations.
How to Master ECGs
Recognizing an R on T premature ventricular complex (PVC) is just one of the skills an ECG reader should have.
If you want to learn to read ECGs or hone your skills, Executive Electrocardiogram Education has a wide range of courses to choose from. Every medical provider can benefit. Continuing Medical Education Credits are also available.
To get a feel for our courses, sign up for our free ACLS Rhythms Course. For a complete ECG interpretation course, check out ECG Premium Course, which includes ECG criteria, a systematic approach to reading ECGs, arrhythmia recognition, and plenty of practice ECGs.



